Clinical
Our clinical nursing articles aim to inform and educate nurse practitioners and students. This is achieved through the publication of peer-reviewed, evidence-based, relevant and topical articles.
Perceptions of the use of terms of endearment among older adults in an assisted living...
Why you should read this article: • To increase your understanding of ‘elderspeak’ and the use of terms of endearment with older adults • To recognise that acceptance or rejection of the use of terms of endearment may be a matter of opinion • To enhance your practice by considering and acknowledging each individual’s communication preferences Background ‘Elderspeak’ has been defined as a form of communication overaccommodation used with older adults that typically involves inappropriate simplified speech. One aspect of elderspeak is the use of terms of endearment such as ‘honey’, sweetie’ and ‘dear’. There is disagreement regarding the use of terms of endearment with older adults, with differing views on whether it is beneficial or harmful. Aim To explore the perceptions of older adults residing in an assisted living facility on the use of terms of endearment by healthcare staff. Method This qualitative study used a descriptive phenomenological design. Semi-structured interviews were undertaken with 15 older adults regarding their perceptions of the use of terms of endearment. The data were analysed to identify themes. Findings Two themes emerged from the interview data: ‘it’s a matter of opinion’ and ‘context matters’. Not all older adults viewed terms of endearment negatively; some liked them, others were neutral and some viewed them as childish or disrespectful. Conclusion Perceptions regarding the use of terms of endearment appear to differ among older adults. Therefore, the use of such terms should be individualised based on the preferences of the older adult.
Risk management and decision-making in dementia care
Encouraging a proactive and person-centred approach to risk assessment and management
Using therapeutic lies – an ethical challenge for nurses
White lies' can be useful when caring for people with dementia, but is it ethical to use them?
Severe frailty diagnosis: advance care planning and end of life care conversations
People with severe frailty may be disadvantaged in terms of receiving appropriate end of life care
Exploring the professional nurse advocate role and restorative clinical supervision
The role aims to provide clinical, educational and well-being support to nurses
Supporting shared decision-making in medicines use with people living with dementia
Shared decision-making may help support people to make informed decisions about their treatment
Equipping the healthcare workforce to meet the needs of older people in the community
Explore the benefits of a versatile, multiskilled workforce for the wider healthcare system
Nurses’ experiences of identifying delirium superimposed on dementia
How aesthetic ways of knowing people can enhance patient assessment
A journal club for healthcare professionals in an older people’s residential setting
Such clubs can help develop staff members’ critical thinking and presentation and communication skills
Music therapy interventions in a dementia inpatient unit: reflections and practicalities
Learning points from therapy sessions including engaging individuals and staff, timing and benefits
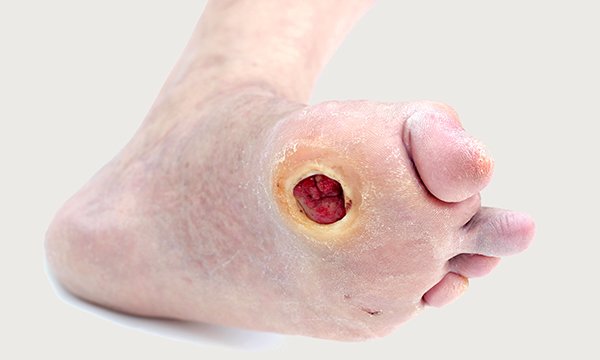
Diabetic foot ulcers in older people: prevention and management
How to avoid the potentially devastating effects of foot ulcers
Who am I? Identity, person-centred care and dementia
Actively seeking a person’s concept of self can help nurses deliver personalised care